TMJ Guide
TMJ vs Bruxism: Key Differences and Treatment (2026)
TMJ vs Bruxism: Key Differences and Treatment (2026) article.
By Dr. Sarah Mitchell · Published 2026-03-12 · Updated 2026-03-12

By Dr. Sarah Mitchell, Orofacial Pain Specialist | Last updated: March 2026
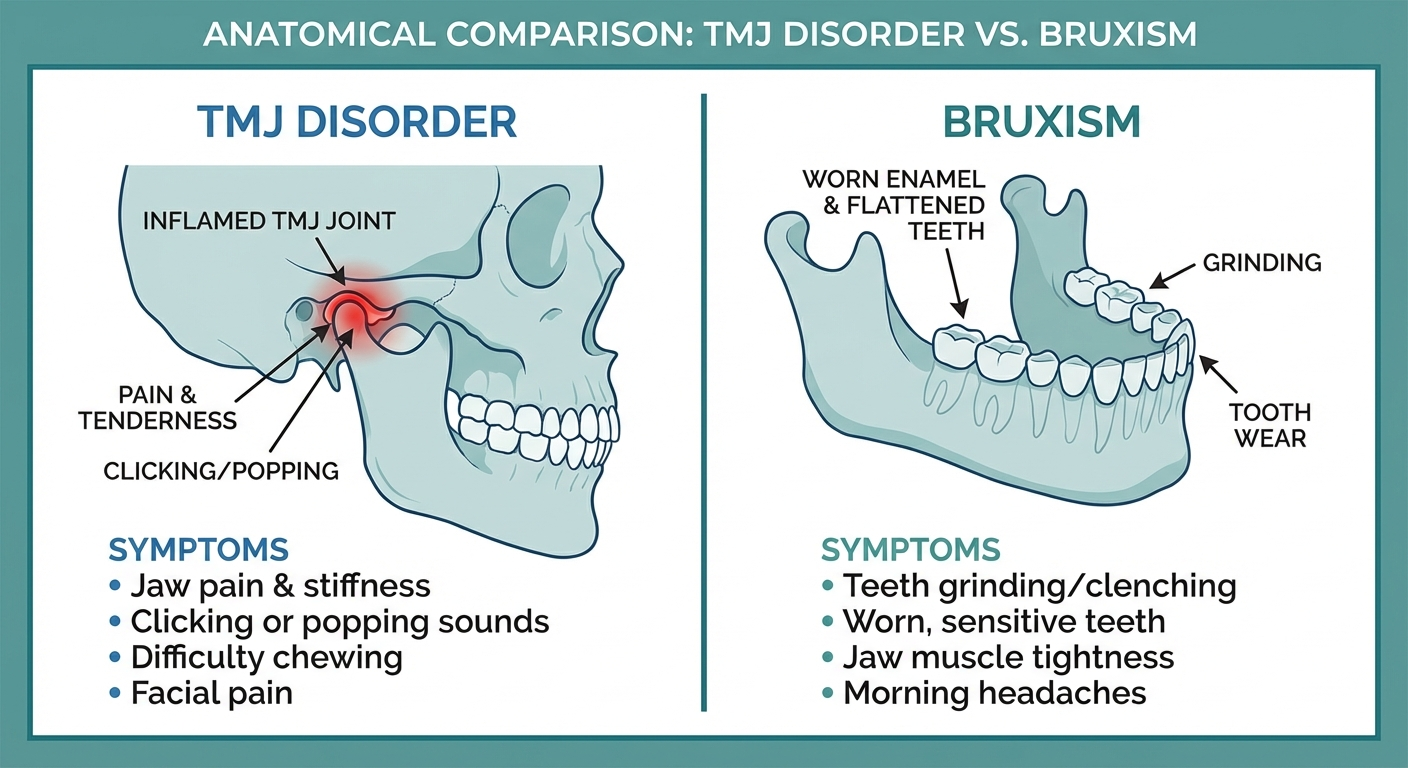
TMJ disorder and bruxism are two distinct but closely related jaw conditions. TMJ disorder (temporomandibular joint disorder) refers to dysfunction of the jaw joint itself — causing pain, clicking, and limited movement. Bruxism is the involuntary habit of grinding or clenching the teeth, often during sleep. While bruxism can cause TMJ disorder, and TMJ disorder can worsen bruxism, they require different diagnostic and treatment approaches.
Table of Contents
![Medical infographic: [person holding jaw in pain from TMJ]](/images/tmj-vs-bruxism-img1.png)
- What Is TMJ Disorder?
- What Is Bruxism?
- Are TMJ Disorder and Bruxism Connected?
- TMJ vs Bruxism: Side-by-Side Comparison
- Treatment Options for TMJ Disorder
- Treatment Options for Bruxism
- Products That Help Both Conditions
- Frequently Asked Questions
- Sources and Methodology
What Is TMJ Disorder?
TMJ disorder — sometimes called TMD or temporomandibular disorder — is a condition affecting the temporomandibular joint, the hinge-like joint that connects your jawbone to your skull on each side of your head. You use this joint every time you chew, speak, or yawn. When something goes wrong with the joint, the surrounding muscles, or the disc inside the joint, the result is pain, dysfunction, and a significant reduction in quality of life.
According to the National Institute of Dental and Craniofacial Research (NIDCR), TMJ disorders affect more than 10 million Americans at any given time. The condition is roughly twice as common in women as in men, with peak prevalence occurring between the ages of 20 and 40.
Common Causes of TMJ Disorder
TMJ disorder rarely has a single cause. Instead, it usually develops from a combination of factors:
- Jaw injury or trauma — a blow to the jaw, whiplash, or even aggressive dental work can damage the joint or displace the articular disc.
- Arthritis — both osteoarthritis and rheumatoid arthritis can affect the temporomandibular joint, breaking down cartilage over time.
- Disc displacement — the small cartilage disc that cushions the joint can slip out of position, causing clicking, popping, or locking.
- Muscle tension and overuse — chronic clenching, poor posture, and stress-related tension in the jaw and neck muscles contribute to TMJ symptoms.
- Malocclusion — a misaligned bite places uneven stress on the jaw joint.
- Genetic predisposition — some individuals have structural variations in the jaw joint that make them more susceptible to TMJ problems.
TMJ Symptoms to Watch For
TMJ disorder presents with a range of symptoms that can vary from mild discomfort to debilitating pain. Here at Jaw Pain Guide, we encourage readers to track their symptoms carefully, as patterns often help clinicians reach an accurate diagnosis.
The most common TMJ symptoms include:
- Jaw pain or tenderness, especially when chewing or speaking
- Clicking, popping, or grating sounds when opening or closing the mouth
- Jaw locking in an open or closed position
- Difficulty opening the mouth wide
- Pain radiating to the ear, temple, or neck
- Facial swelling on the affected side
- Headaches, particularly upon waking
- Changes in how the upper and lower teeth fit together
According to the Mayo Clinic, TMJ pain is often temporary and can be resolved with self-care and nonsurgical treatments. However, some patients experience chronic symptoms that require more advanced intervention.
Who Gets TMJ Disorder?
Research published by the American Dental Association (ADA) indicates that TMJ disorders disproportionately affect women of reproductive age, suggesting a potential hormonal component. Other high-risk groups include individuals with chronic stress, those with a history of jaw trauma, people with autoimmune conditions affecting the joints, and patients who grind or clench their teeth habitually.
What Is Bruxism?
![[dentist examining patient jaw for TMJ diagnosis]](/images/tmj-vs-bruxism-img2.png)
Bruxism is the medical term for involuntary teeth grinding or jaw clenching. It can occur during the day (awake bruxism) or during sleep (sleep bruxism), and many people who have bruxism are entirely unaware of the habit until a dentist notices telltale signs of enamel wear or a partner reports hearing grinding sounds at night.
According to the American Sleep Association, sleep bruxism affects approximately 8% of adults, though the actual number may be higher due to underdiagnosis. When both awake and sleep bruxism are considered, studies published in the Journal of Oral Rehabilitation suggest that bruxism affects roughly 31% of adults to some degree — making it one of the most common oral health conditions worldwide.
Common Causes of Bruxism
Bruxism is a multifactorial condition. The major contributing factors include:
- Stress and anxiety — emotional tension is the single most commonly cited trigger for awake bruxism, and it is strongly associated with sleep bruxism as well.
- Sleep disorders — obstructive sleep apnea (OSA) is closely linked to sleep bruxism. According to the National Institutes of Health (NIH), individuals with OSA are significantly more likely to grind their teeth during sleep.
- Medications — certain antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), can trigger or worsen bruxism as a side effect.
- Lifestyle factors — high caffeine intake, alcohol use, tobacco use, and recreational drug use are all associated with increased bruxism risk.
- Malocclusion — while the evidence is debated, some research suggests that bite misalignment can contribute to grinding habits.
- Genetics — sleep bruxism tends to run in families, with studies showing a higher concordance rate among identical twins.
Bruxism Symptoms
Unlike TMJ disorder, bruxism symptoms are often subtle in the early stages. Many patients first learn they grind their teeth during a routine dental exam. Key bruxism symptoms include:
- Audible teeth grinding during sleep (reported by a sleep partner)
- Worn, flattened, or chipped teeth
- Tooth sensitivity or unexplained toothaches
- Jaw soreness or fatigue, especially in the morning
- Dull headaches originating at the temples
- Cheek biting or tongue indentations
- Tight or tired jaw muscles
- Disrupted sleep
Who Gets Bruxism?
Bruxism does not discriminate by age or gender as strongly as TMJ disorder does. According to the ADA, bruxism is common in children (who often outgrow it), adults under significant stress, individuals taking certain psychiatric medications, and those with sleep-disordered breathing. However, the condition is observed across all demographics.
Are TMJ Disorder and Bruxism Connected?
Yes — and understanding the bidirectional relationship between TMJ disorder and bruxism is critical for effective treatment. At Jaw Pain Guide, we frequently see readers who have been diagnosed with one condition but actually have both, which is why proper differential diagnosis matters so much.
Bruxism as a Cause of TMJ Disorder
Chronic teeth grinding and clenching places enormous mechanical stress on the temporomandibular joint. The masseter muscle — the primary chewing muscle — can generate forces exceeding 250 pounds per square inch during bruxism episodes. Over time, this repetitive overloading can cause inflammation of the joint capsule, displacement of the articular disc, muscle fatigue and myofascial pain, and accelerated wear of the cartilage surfaces within the joint.
A 2019 systematic review published in the Journal of Oral & Facial Pain and Headache found that individuals with sleep bruxism were 2.5 to 4 times more likely to develop TMJ disorder symptoms compared to non-bruxers. This makes bruxism one of the most significant modifiable risk factors for TMJ disorder.
TMJ Disorder as a Contributor to Bruxism
The relationship works in the other direction too. Patients with TMJ disorder may develop compensatory grinding or clenching patterns as the brain unconsciously attempts to find a more comfortable jaw position. Pain-related sleep fragmentation from TMJ disorder can also trigger sleep bruxism episodes, and the stress and anxiety that often accompany chronic TMJ pain can further drive awake bruxism habits.
According to research cited by the NIH, patients with existing TMJ disorder who develop bruxism experience faster disease progression and more severe pain outcomes than those with TMJ disorder alone. This creates a vicious cycle where each condition perpetuates the other, making early and simultaneous treatment of both conditions essential.
TMJ vs Bruxism: Side-by-Side Comparison
![[close-up of teeth showing signs of grinding/bruxism wear]](/images/tmj-vs-bruxism-img3.png)
The following comparison table summarizes the key differences between bruxism vs TMJ disorder across the most important clinical dimensions:
| Feature | TMJ Disorder | Bruxism |
|---|---|---|
| Definition | Dysfunction of the temporomandibular joint and surrounding structures | Involuntary grinding or clenching of the teeth |
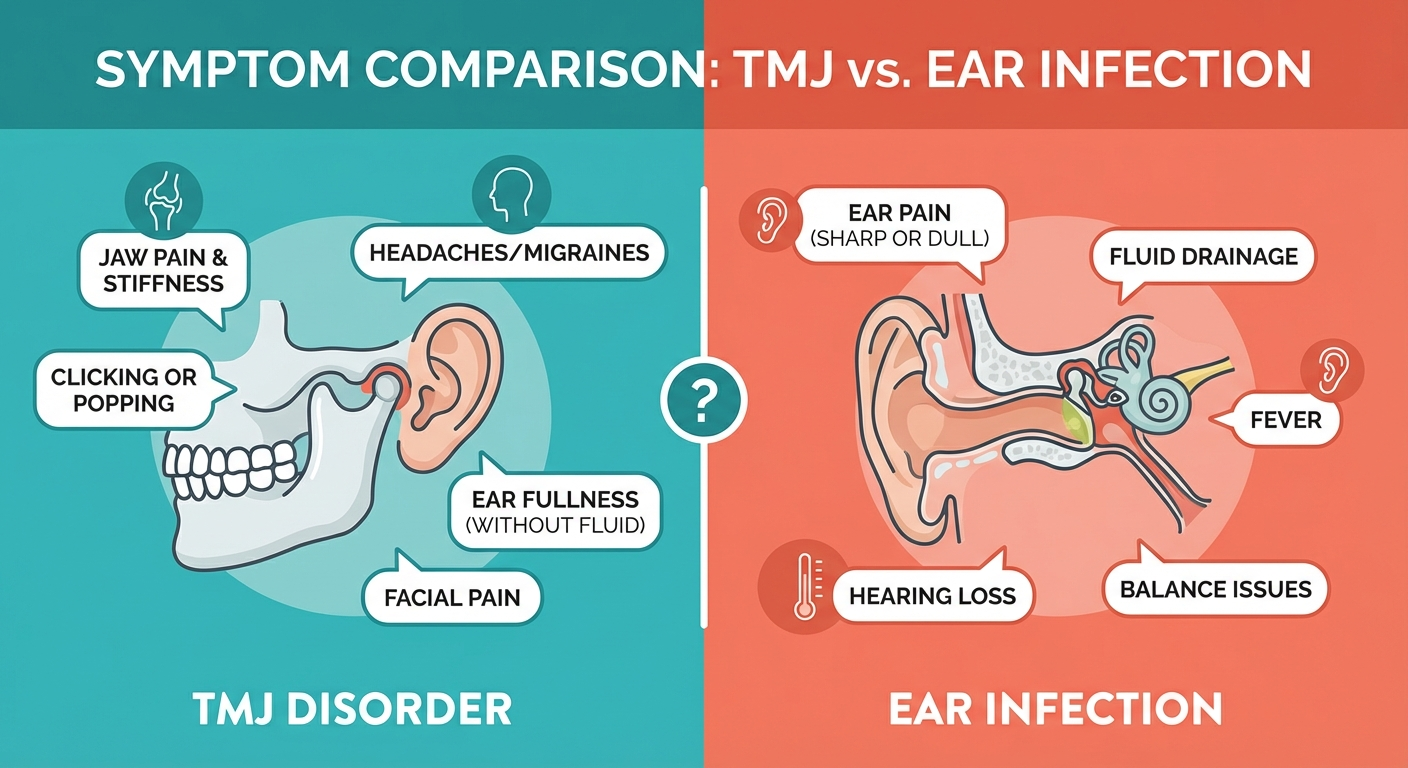
| Primary Symptoms | Jaw pain, clicking/popping, limited jaw movement, ear pain | Worn/damaged teeth, morning jaw soreness, headaches |
| Common Causes | Injury, arthritis, disc displacement, muscle tension | Stress, sleep disorders, medications, lifestyle factors |
| Risk Factors | Female sex, age 20–40, jaw trauma, autoimmune conditions | Stress, sleep apnea, SSRI use, caffeine/alcohol |
| Diagnosis Method | Clinical exam, imaging (X-ray, MRI, CT), joint palpation | Dental exam (enamel wear), sleep study, EMG |
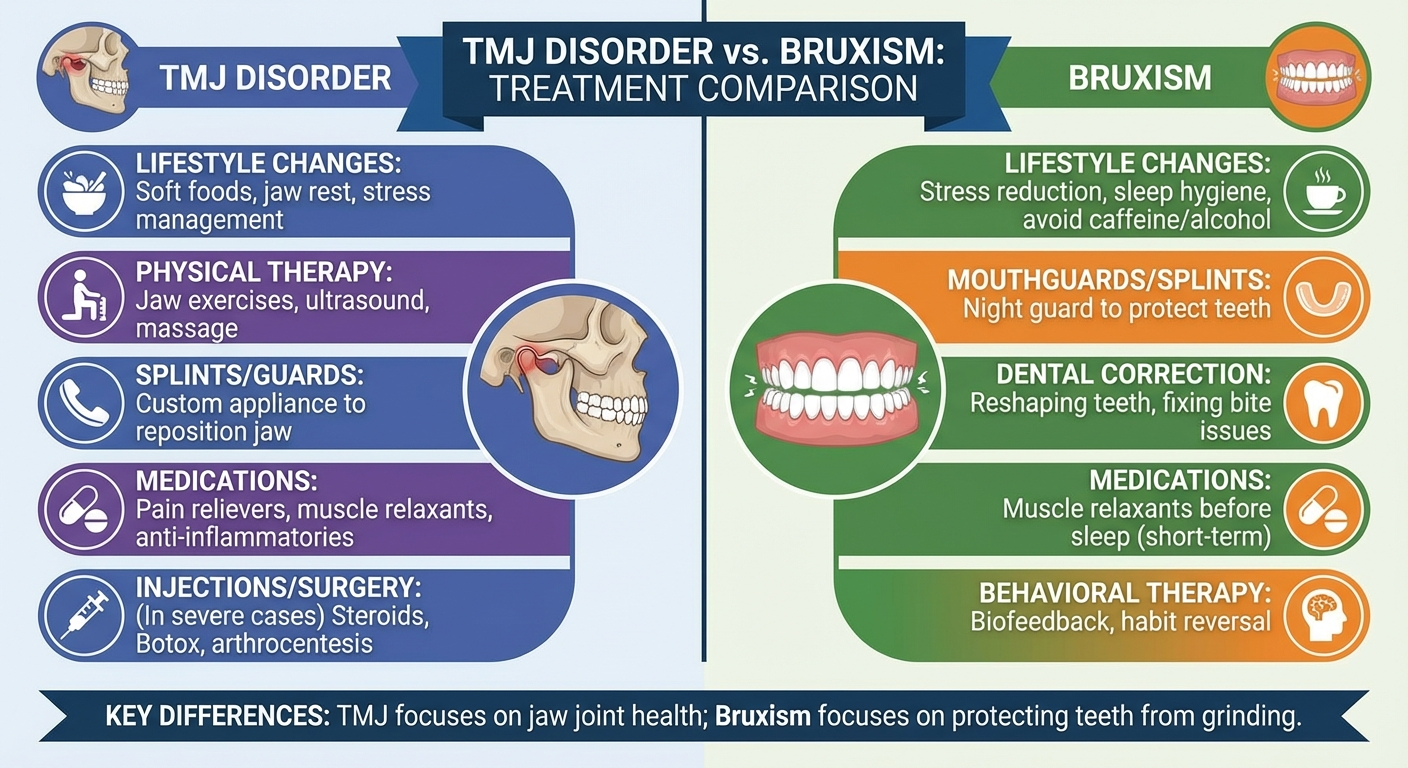
| Primary Treatment | Physical therapy, splints, anti-inflammatories, surgery (last resort) | Night guards, stress management, Botox, biofeedback |
| When to See a Doctor | Persistent jaw pain, locking, difficulty eating or speaking | Visible tooth damage, partner reports grinding, chronic headaches |
This table highlights that while bruxism vs TMJ share some overlapping symptoms — particularly jaw soreness and headaches — they are fundamentally different conditions with different root causes and treatment strategies.
Treatment Options for TMJ Disorder
TMJ disorder treatment follows a conservative-first philosophy. Most clinical guidelines recommend starting with the least invasive interventions and escalating only when symptoms persist. For a deeper dive into home-based strategies, see our guide on TMJ Treatment at Home.
Jaw Exercises and Physical Therapy
Targeted jaw exercises are a cornerstone of TMJ disorder management. A trained physical therapist specializing in orofacial pain can design a program that includes jaw stretching and range-of-motion exercises, manual therapy to release tight muscles and fascial restrictions, postural correction (especially for forward head posture), and dry needling or trigger point therapy for myofascial pain.
According to the ADA, physical therapy produces measurable improvement in jaw function and pain reduction in the majority of TMJ disorder patients within 4 to 6 weeks.
Oral Appliances and Mouth Guards
Stabilization splints (also called occlusal splints or bite guards) are frequently prescribed for TMJ disorder. These custom-fitted devices reposition the jaw to reduce stress on the joint, prevent tooth contact during clenching episodes, and allow the muscles of mastication to relax. A well-fitted TMJ mouth guard can provide significant relief. For product recommendations, visit our guide on the Best Mouth Guard for TMJ.
Medications
Several classes of medication can help manage TMJ symptoms:
- NSAIDs (ibuprofen, naproxen) — reduce inflammation and pain
- Muscle relaxants (cyclobenzaprine) — relieve jaw muscle spasm, especially at night
- Tricyclic antidepressants (amitriptyline, at low doses) — modulate chronic pain signaling
- Corticosteroid injections — reduce severe joint inflammation in acute flare-ups
Surgical Options (Last Resort)
Surgery for TMJ disorder is reserved for cases that fail to respond to conservative treatment over 3 to 6 months. Options include arthrocentesis (joint lavage), arthroscopy (minimally invasive joint surgery), and open-joint surgery (arthroplasty or joint replacement). The NIDCR advises that irreversible surgical procedures should be avoided whenever possible, as outcomes are variable and complications can occur.
Treatment Options for Bruxism

Treating bruxism effectively requires addressing the grinding behavior itself, its underlying causes, and any damage already done to the teeth and jaw.
Night Guards and Occlusal Splints
Custom night guards remain the most widely recommended treatment for sleep bruxism. These devices do not stop the grinding habit itself, but they protect the teeth from further wear, reduce the forces transmitted to the temporomandibular joint, and minimize morning jaw soreness and headaches. Over-the-counter boil-and-bite guards can serve as a temporary solution, but custom guards from a dentist offer superior fit, comfort, and durability.
Stress Management
Because stress is the primary driver of awake bruxism and a major contributor to sleep bruxism, stress reduction strategies are an essential component of treatment:
- Cognitive behavioral therapy (CBT) — helps patients identify and modify clenching habits and manage the anxiety and tension that trigger them
- Mindfulness and meditation — regular practice has been shown to reduce muscle tension and improve awareness of clenching during the day
- Progressive muscle relaxation — targeted relaxation of the jaw and facial muscles before sleep can reduce nocturnal grinding
- Exercise — regular physical activity is one of the most effective stress-reduction tools available
Botox Injections
Botulinum toxin (Botox) injections into the masseter and temporalis muscles have emerged as an effective treatment for severe bruxism that does not respond to conservative measures. According to research published in the Journal of Dental Research, Botox reduces grinding force by 30% to 50% and provides relief for approximately 3 to 4 months per treatment cycle. While not yet FDA-approved specifically for bruxism, Botox is used off-label by many orofacial pain specialists.
Biofeedback
Biofeedback therapy uses sensors placed on the jaw muscles to detect clenching in real time, providing auditory or visual alerts that help the patient become aware of and consciously relax their jaw. Biofeedback is particularly effective for awake bruxism. Wearable biofeedback headbands designed for nighttime use are also gaining traction, though evidence for their long-term effectiveness is still evolving.
Dental Correction
In cases where bite misalignment is contributing to bruxism, orthodontic treatment or dental restorations may be recommended. However, most experts caution against aggressive, irreversible dental procedures for bruxism unless there is clear evidence that malocclusion is a contributing factor.
Addressing Underlying Sleep Disorders
Because sleep bruxism is closely linked to obstructive sleep apnea, patients with suspected sleep-disordered breathing should be evaluated with a polysomnography (sleep study). Treating OSA with CPAP therapy, a mandibular advancement device, or other interventions often reduces or eliminates concurrent sleep bruxism.
Products That Help Both Conditions
Many of the same products can provide relief for both TMJ disorder and bruxism. Here at Jaw Pain Guide, we recommend the following categories based on evidence and reader feedback:
Mouth Guards and Occlusal Splints
A quality mouth guard protects teeth from grinding damage while simultaneously reducing stress on the temporomandibular joint. Custom options from a dentist are ideal, but over-the-counter guards can be a good starting point.
Jaw Exercisers
Jaw exercise tools made from food-grade silicone can help strengthen and stretch the muscles of mastication, benefiting both TMJ disorder rehab and bruxism-related muscle fatigue. Use them gently and according to your provider's instructions.
Heat and Cold Therapy Packs
Moist heat packs increase blood flow and relax tight jaw muscles, while cold packs reduce acute inflammation. Many TMJ and bruxism patients find alternating heat and cold to be one of the simplest and most effective home remedies.
Magnesium Supplements
Magnesium plays a role in muscle relaxation and nerve function. Some studies suggest that magnesium supplementation may reduce nighttime teeth grinding, though more research is needed. Consult your healthcare provider before starting any supplement regimen.
Stress Relief and Relaxation Aids
Products such as weighted blankets, acupressure mats, and aromatherapy diffusers can support the stress-management component of both TMJ and bruxism treatment plans.
Frequently Asked Questions
Is bruxism the same as TMJ?
No, bruxism and TMJ disorder are not the same condition. Bruxism refers specifically to the habit of grinding or clenching the teeth, while TMJ disorder is a condition affecting the temporomandibular joint itself. However, the two conditions are closely related, and bruxism is one of the leading risk factors for developing TMJ disorder.
Can bruxism cause TMJ disorder?
Yes. Chronic teeth grinding and clenching places excessive mechanical stress on the temporomandibular joint, which can lead to joint inflammation, disc displacement, and muscle fatigue — all hallmarks of TMJ disorder. Research shows that individuals with bruxism are 2.5 to 4 times more likely to develop TMJ disorder symptoms compared to non-bruxers.
How do I know if I have TMJ or bruxism?
The key distinguishing factors are symptom location and type. TMJ disorder typically presents with jaw joint pain, clicking or popping sounds, and limited jaw movement. Bruxism is characterized by worn or damaged teeth, morning jaw soreness, and headaches. A dentist or orofacial pain specialist can provide a definitive diagnosis using clinical examination, dental assessment, and imaging studies when needed.
Can you have both TMJ and bruxism?
Absolutely. Having both TMJ disorder and bruxism simultaneously is quite common. The two conditions share a bidirectional relationship — bruxism can cause or worsen TMJ disorder, and the pain and dysfunction of TMJ disorder can trigger or intensify bruxism. When both conditions are present, treating them concurrently produces the best outcomes.
What doctor treats TMJ and bruxism?
Several types of healthcare providers can diagnose and treat TMJ disorder and bruxism. Your general dentist is often the first point of contact. For more complex cases, you may be referred to an orofacial pain specialist, an oral and maxillofacial surgeon, a TMJ-focused physical therapist, or a sleep medicine physician (especially if sleep bruxism is linked to a sleep disorder).
Does insurance cover TMJ and bruxism treatment?
Coverage varies significantly by plan. Many dental insurance plans cover night guards and basic splint therapy. Medical insurance may cover physical therapy, imaging, and surgical procedures for TMJ disorder when deemed medically necessary. Contact your insurance provider for specifics regarding your plan's coverage for TMJ disorders and bruxism treatment.
Sources and Methodology
This article was researched and written by Dr. Sarah Mitchell for Jaw Pain Guide using evidence from the following authoritative sources:
- National Institute of Dental and Craniofacial Research (NIDCR) — prevalence data on TMJ disorders and treatment guidelines. nidcr.nih.gov
- American Dental Association (ADA) — clinical recommendations for bruxism management and oral appliance therapy. ada.org
- National Institutes of Health (NIH) — research on the relationship between sleep bruxism, obstructive sleep apnea, and TMJ disorders. nih.gov
- Mayo Clinic — patient education resources on TMJ disorder symptoms, diagnosis, and treatment options. mayoclinic.org
- American Sleep Association — data on sleep bruxism prevalence and its relationship to sleep disorders. sleepassociation.org
All statistics cited in this article are drawn from peer-reviewed research, government health agencies, or established medical organizations. Content is reviewed and updated regularly to reflect the latest clinical evidence.
Medical Disclaimer
The information provided on Jaw Pain Guide is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding TMJ disorder, bruxism, or any other medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. If you are experiencing severe jaw pain, difficulty breathing, or chest pain, seek emergency medical attention immediately.
Visual Guide Gallery
Walking Pad vs Treadmill
30-second comparison