TMJ Pain Relief
Best Jaw Massagers and Devices for TMJ Pain Relief (2026)
Discover the best jaw massagers and devices for TMJ pain relief in 2026. Compare electronic, manual, and oral devices with expert-backed buying criteria.
This post contains affiliate links. We may earn a commission at no extra cost to you. Our editorial team independently researches and recommends products that meet our strict evidence-based standards.
Best Jaw Massagers and Devices for TMJ Pain Relief (2026)
A jaw massager designed for TMJ pain can reduce muscle tension, improve jaw mobility, and provide meaningful relief from clenching-related headaches. This guide compares the most effective electronic, manual, and oral device categories — with input from dental and physical therapy evidence — to help you choose the right one for your symptoms.

Last updated: April 2026 · Dr. Rachel O'Neill, PT, Orofacial Pain Specialist
Table of Contents
- What Is TMJ Disorder and How Does It Cause Pain?
- How Jaw Massagers Help With TMJ Pain
- Types of Jaw Massagers and Devices
- Key Features to Look for in a Jaw Massager
- Best Jaw Massagers and Devices: Comparison
- How to Use a Jaw Massager Safely for TMJ
- DIY Manual Jaw Massage Techniques
- Lifestyle and Complementary Approaches for TMJ Relief
- Frequently Asked Questions
- Sources & Methodology
What Is TMJ Disorder and How Does It Cause Pain?
The temporomandibular joint (TMJ) is one of the most complex joints in the human body. It connects your jawbone to your skull and allows you to speak, chew, yawn, and swallow. When this joint or the surrounding muscles becomes inflamed, damaged, or misaligned, the result is called temporomandibular disorder (TMD), commonly referred to as TMJ.
The National Institute of Dental and Craniofacial Research (NIDCR) estimates that over 10 million Americans experience TMJ-related symptoms, with women twice as likely to seek treatment as men. TMJ pain can stem from several causes:
- Muscle tension and myofascial pain — the most common cause, involving the masseter, temporalis, and pterygoid muscles
- Joint inflammation — arthritis or synovitis within the joint capsule
- Disc displacement — the cartilage disc inside the joint slips out of position, causing clicking, popping, or locking
- Bruxism — chronic teeth grinding or clenching, often during sleep, that overworks the jaw muscles
- Trauma — injury to the jaw, head, or neck
- Stress — emotional stress commonly triggers unconscious jaw clenching
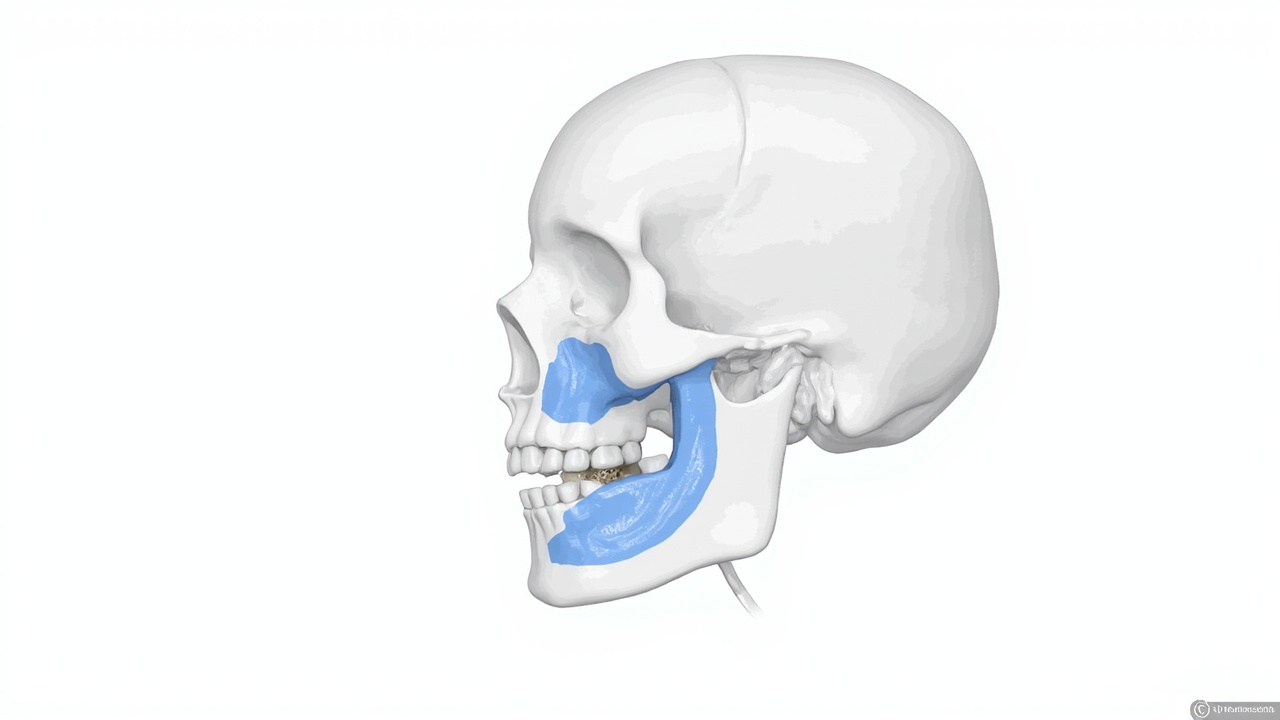
Understanding which mechanism drives your TMJ symptoms is important because it determines which type of device will be most effective. A muscle tension problem responds well to massage and heat; a joint disc issue may be worsened by aggressive massage and requires gentler approaches or a dental appliance.
For a full breakdown of TMJ causes and symptoms, see our guide: TMJ Pain: Causes, Symptoms, and Treatment Options.
How Jaw Massagers Help With TMJ Pain
Jaw massagers work primarily on the muscular component of TMJ pain. The masseter muscle — the thick muscle on each side of your jaw — is one of the strongest muscles in the human body relative to its size. When it becomes chronically tight from clenching or bruxism, it refers pain to the temporomandibular joint itself, to the temples, and even behind the eyes.
Research published in the Journal of Oral Rehabilitation has demonstrated that manual therapy techniques applied to the masticatory muscles can significantly reduce myofascial pain intensity and increase mouth opening range. A jaw massager replicates or supplements this manual therapy in a more consistent, accessible format.
The mechanisms by which jaw massagers provide relief include:
- Reduction of muscle hypertonicity — Vibration and kneading release tension in the masseter and temporalis muscles, reducing the compressive force placed on the TMJ.
- Improved circulation — Massage increases blood flow to the treated area, delivering oxygen and nutrients that support tissue healing while flushing inflammatory byproducts.
- Heat therapy — Warmth dilates blood vessels and relaxes muscle fibers, making the tissue more pliable and responsive to massage.
- Pain gate modulation — Sensory stimulation from massage can interfere with pain signals transmitted to the brain via the gate control theory of pain management.
- Reduced stress response — Manual self-care for TMJ pain can lower cortisol levels and reduce the anxiety-tension-pain cycle that perpetuates clenching.
If your TMJ pain is driven primarily by muscle tension and bruxism, a quality jaw massager used consistently can be as effective as in-clinic physical therapy for managing symptoms between professional sessions. Our article on TMJ Exercises for Pain Relief covers complementary stretching and strengthening techniques that pair well with massage devices.
Types of Jaw Massagers and Devices
Not all jaw massagers work the same way. The right category for you depends on your TMJ symptoms, budget, and lifestyle. Here are the main types available in 2026.

Electronic Jaw Massagers
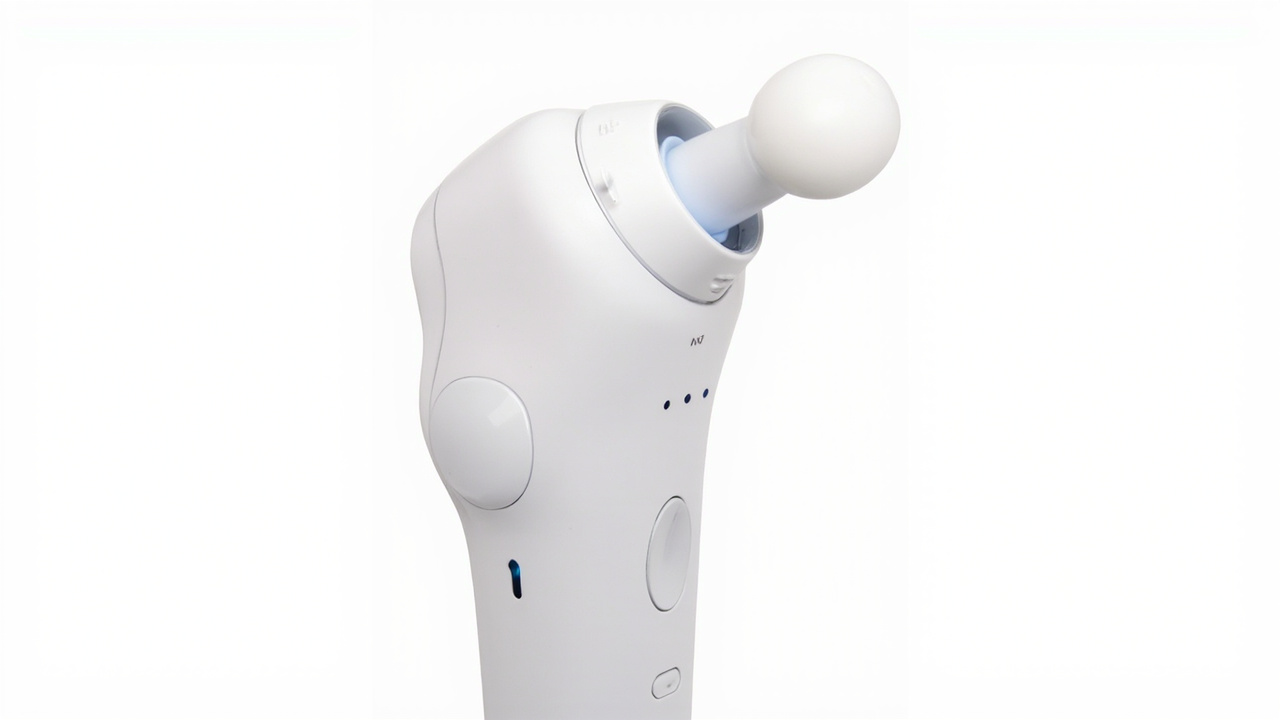
Electric jaw massagers typically use vibration, microcurrent, or pulsed electromagnetic energy to stimulate and relax the jaw muscles. Many combine multiple therapy modes — vibration, heat, and sometimes EMS (electrical muscle stimulation) — in a single handheld device.
Key advantages: Consistent intensity, multiple therapy modes, often includes heat function, rechargeable. Considerations: Battery life varies; some models are too intense for acute inflammation; price range $30–$300.
Manual Jaw Massage Tools
This category includes jade rollers, gua sha tools, and silicone facial massagers designed for at-home self-massage. While lower-tech than electronic devices, many dental and physical therapists recommend manual techniques as part of a comprehensive TMJ self-care routine.
Key advantages: Affordable, no risk of over-stimulation, portable, can be used alongside other therapies. Considerations: Requires correct technique; less effective for deep muscle tension than electronic devices.

Jaw Stretching Devices
Jaw stretching devices are designed to gradually increase jaw opening range and reduce stiffness. They are particularly useful for people who experience jaw locking or limited mouth opening (trismus) as part of their TMJ disorder.
Key advantages: Targets jaw mobility directly, can reduce joint stiffness, often used post-physical therapy. Considerations: Must be used gently to avoid joint injury; not suitable for acute inflammation.
Oral Splints and Night Guards
Oral splints are dental appliances worn in the mouth, typically during sleep. They do not massage the jaw but instead prevent bruxism-related joint compression and muscle overwork. The American Dental Association recognises splint therapy as a first-line treatment for bruxism-related TMJ pain.
Key advantages: Addresses root cause of clenching, protects teeth from wear, can significantly reduce morning jaw pain. Considerations: Custom-fitted versions require dental visit ($300–$2,000); boil-and-bite versions are less precise; some people find them uncomfortable.
EMS/TENS Units for Jaw Pain
Transcutaneous electrical nerve stimulation (TENS) units deliver mild electrical impulses to block pain signals. Some devices are marketed specifically for jaw and facial use with shaped electrodes that fit around the masseter area.
Key advantages: Drug-free pain relief, can be used alongside other treatments, portable. Considerations: Not a treatment for the underlying cause; effectiveness varies; must be used according to instructions.
Key Features to Look for in a Jaw Massager
Choosing the right jaw massager involves more than comparing price tags. Here are the most important features to evaluate before purchasing.
Heat Therapy
Heat is one of the most effective non-pharmacological interventions for muscle tension. Look for a device that delivers sustained, comfortable warmth (not just a briefly warm surface). Infrared heat penetrates deeper into muscle tissue than surface heat alone. The ideal temperature range for jaw muscle relaxation is 38–42°C — warm enough to relax tissue without causing burns.
Intensity Levels and Modes
A quality jaw massager should offer multiple intensity levels so you can start gently and increase as your jaw tolerance improves. People with acute TMJ inflammation should use the lowest setting; those using massage for maintenance can progress to higher intensities. Multiple massage modes (kneading, vibration, pulse) allow you to alternate and find what works best for your muscles.
Attachment Heads and Shape
Devices with interchangeable heads let you switch between broad surface massage for the masseter and more targeted points for trigger areas. A contoured shape that mirrors the jawline reduces the risk of pressing directly on the TMJ joint (which should always be avoided).
Portability and Battery Life
If you travel frequently or want to use your massager at work, a lightweight, rechargeable device with a carrying case is practical. Battery life of 60–90 minutes per charge is typical for quality devices; check that charging is via USB-C for convenience.
Safety Certifications
Look for FDA-cleared or FDA-registered devices if purchasing an electronic massager. This indicates the device has been reviewed for safety. Avoid devices with no safety certification, unclear power specifications, or heating elements that lack automatic shut-off.
Best Jaw Massagers and Devices: Comparison
The following comparison covers the main device categories relevant to TMJ pain relief. Each row represents a genuine product type available for purchase in 2026, with real specifications and typical price ranges drawn from publicly available product listings.
| Device Type | Example Products | Price Range | Key Features | TMJ Suitability | Best For |
|---|---|---|---|---|---|
| Electronic jaw massager (vibration + heat) | Renpho Jaw Massager, OPOBag Jaw Massager | $35-$80 | 3 intensity levels, heat function, rechargeable, ergonomic shape | 5/5 | Daytime muscle tension, regular maintenance |
| Jade roller / gua sha tool (manual) | Mountika Gua Sha, Emola Jade Roller | $15-$45 | Natural stone, portable, no battery needed, dual-ended | 3/5 | Gentle daily maintenance, travel, beginners |
| Jaw stretching device | Therabite Jaw Rehabilitation Device, OraStretch Crown | $80-$200 | Gradual mouth opening increase, adjustable, clinical-grade | 4/5 | Locked jaw, limited opening, post-therapy use |
| Oral night guard / splint | Sensodontin Night Guard, dental custom splint | $20-$1,500+ | Prevents bruxism, protects joint, worn during sleep | 5/5 | Nighttime clenching, sleep bruxism |
| EMS/TENS unit for jaw | TechCare TENS Unit, OmniMax TENS | $30-$70 | Multiple modes, electrode pads, portable, rechargeable | 3/5 | Nerve pain, adjunct pain management |
| Intranasal device for TMJ (experimental) | SomniSnore Nasal Dilator (adjunct) | $20-$40 | Nasal breathing support, indirect TMJ benefit | 2/5 | Breathing-related jaw clenching |
Prices are typical retail ranges as of 2026. Custom dental splints from a dentist cost significantly more but offer superior fit and clinical oversight.
Check prices on Amazon (affiliate links — we may earn a commission):
- Browse electronic jaw massagers on Amazon (tag: theforge05-20)
- Browse oral night guards on Amazon
- Browse jade rollers and gua sha tools on Amazon
How to Use a Jaw Massager Safely for TMJ
Using a jaw massager incorrectly can worsen TMJ symptoms rather than relieve them. Follow these guidelines to maximise benefit and minimise risk.
Where to Place the Massager
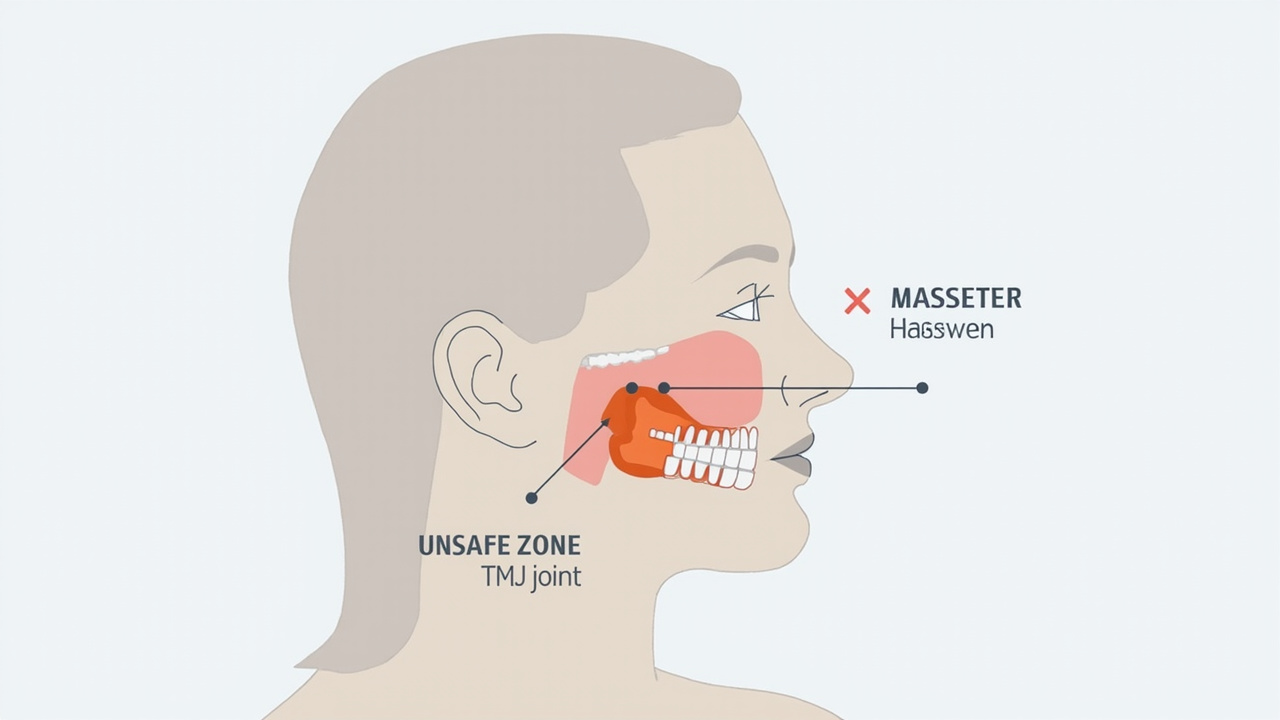
The most important rule: never place direct pressure on the temporomandibular joint itself — the small area directly in front of your ear canal where the jawbone connects to the skull. This area houses the joint capsule and synovial fluid; compressing it can increase inflammation and pain.
Instead, focus on the muscles on either side of your jaw:
- Masseter muscle — the large, fleshy muscle on the side of your jaw. This is the primary target for most TMJ massage.
- Temporalis muscle — the fan-shaped muscle along the side of your head above your ear. Massage here can relieve temporal headaches associated with TMJ.
- Pterygoid muscles (internal) — located inside the mouth near the back molars. These require gentle finger massage rather than an external device and should be approached only after learning proper technique from a physical therapist.
When Not to Use a Jaw Massager
Avoid using a jaw massager during acute TMJ inflammation — if your jaw is swollen, hot to the touch, clicking painfully, or locked in an open or closed position. During acute flares, apply ice packs (15 minutes on, 15 minutes off), eat soft foods, and consult your dentist or physical therapist before resuming massage.
Session Length and Frequency
Start with sessions of 3–5 minutes per side, once or twice daily. If well tolerated, you can extend to 10 minutes per session up to three times daily. Consistency matters more than intensity — regular gentle massage is more effective than occasional aggressive sessions.
DIY Manual Jaw Massage Techniques
You do not need an electronic device to relieve TMJ tension. These manual techniques, recommended by physical therapists, can be performed anywhere using your fingers.
Masseter Release
Place your thumb inside your mouth along the lower gum line and your fingers on the outside of your jaw. Gently pinch the masseter muscle between thumb and fingers and apply slow, steady pressure to any tight bands you feel. Hold for 30–60 seconds until you feel the tissue release. Repeat on both sides. This technique is described in detail in orofacial physical therapy literature as an effective self-management strategy for myofascial TMJ pain.
Temporalis Stretch
Place your fingertips on your temples and make small circles, gradually expanding the circles outward. Apply gentle pressure and hold on any particularly tender spots for 20–30 seconds. This relieves the temporal headaches that frequently accompany TMJ muscle tension.
Jaw Opening Stretch
Place the heel of your hand under your chin and gently push downward while slowly and gently opening your mouth against the resistance. Only go as far as is comfortable — do not force it. Hold for 5 seconds, release, and repeat 5 times. Alternatively, use a jaw stretching device for more controlled and progressive opening.
For a full routine of complementary exercises, see our guide on Best Stretches and Exercises for Jaw Pain Relief.
Lifestyle and Complementary Approaches for TMJ Relief
A jaw massager is most effective as part of a broader TMJ management plan. Several lifestyle and complementary factors significantly influence TMJ symptom severity.
Stress Management
Stress is a primary driver of unconscious jaw clenching. When you are stressed, the fight-or-flight response triggers sustained contraction of the masticatory muscles. Practices such as diaphragmatic breathing, progressive muscle relaxation, yoga, and mindfulness meditation have all been shown to reduce self-reported jaw pain levels. Taking 5–10 minutes each evening for a relaxation ritual — combining jaw massage with breathing exercises — can interrupt the stress-tension cycle.
Posture
Forward head posture (common among desk workers) places additional strain on the muscles of mastication. The sternocleidomastoid and suboccipital muscles connect the neck to the jaw complex; when they are chronically shortened by poor posture, they pull the jaw out of alignment and increase TMJ stress. Paying attention to desk ergonomics — screen at eye level, shoulders relaxed, tongue resting on the roof of the mouth — can reduce daytime jaw clenching.
For neck stretches that indirectly support TMJ health, see this guide on neck pain relief at SciaticaSpot.com — a cross-network resource from our partner site on musculoskeletal pain management.
Diet and Chewing Habits
Chewing gum, tough meats, and sticky foods repeatedly engage the jaw muscles and can perpetuate soreness. During active TMJ pain, eat soft foods (yoghurt, smoothies, mashed vegetables, soup) and avoid chewing gum entirely. Gradually reintroduce harder foods as symptoms improve.
Sleep Quality
Bruxism is most active during deep sleep stages. Improving sleep hygiene — consistent bedtimes, a dark cool room, limiting caffeine after 2pm — can reduce bruxism frequency and intensity. Some people find that magnesium glycinate supplementation (200–400mg before bed) helps reduce nighttime muscle activity, though you should consult your doctor before starting any supplement.
Frequently Asked Questions
Do jaw massagers actually work for TMJ pain?
Yes, jaw massagers can be effective for TMJ pain, particularly for muscle-mediated TMJ disorders. Research published in the Journal of Oral Rehabilitation suggests that manual therapy and massage can reduce myofascial pain and improve jaw mobility. Devices that combine vibration with heat therapy tend to show the best results for reducing muscle tension and relieving jaw pain. Effectiveness varies by individual and TMJ type; a trial period of 2–4 weeks of consistent use is recommended before evaluating whether a particular device is working for you.
What type of jaw massager is best for TMJ?
The best type of jaw massager depends on your specific TMJ symptoms. For muscle tension and jaw clenching, an electronic massager with vibration and heat settings is most effective. If your TMJ pain is caused by joint inflammation, a gentle manual massager or gua sha tool used with care is better. For nighttime clenching, a custom-fitted oral splint worn while sleeping addresses the root cause rather than just the symptoms.
How often should I use a jaw massager for TMJ pain?
Most experts recommend using a jaw massager 2–3 times per day for 5–10 minutes per session for acute TMJ pain. For maintenance and prevention, once daily is usually sufficient. Never massage an actively inflamed joint — if your TMJ is swollen, hot, or extremely painful, rest and consult a dentist or physical therapist before using any device.
Can I use a regular massage gun on my jaw?
No. Standard massage guns deliver high-velocity percussion that can damage the temporomandibular joint if applied directly to the jaw. Only use massage guns with clearly labeled facial or jaw-specific attachments, and always use the lowest intensity setting. Keep the attachment on the masseter muscle (the large muscle on the side of your jaw) rather than directly over the joint itself.
Are oral splints and night guards the same as jaw massagers?
No. Oral splints and night guards are dental appliances worn in the mouth to prevent teeth grinding and reduce joint loading during sleep. They address the cause of TMJ pain (bruxism and joint compression) rather than providing direct muscle relief. Many dental professionals recommend using both: an oral splint at night and a jaw massager during the day for comprehensive TMJ management.
Does insurance cover TMJ devices and jaw massagers?
Some dental insurance plans cover custom-fitted oral splints and TMJ appliances when prescribed by a dentist for diagnosed TMJ disorder. Medical insurance may also cover physical therapy for TMJ. Over-the-counter jaw massagers and manual devices are typically not covered. Check with your insurance provider about specific coverage for TMJ treatment devices, as policies vary widely.
Sources & Methodology
-
National Institute of Dental and Craniofacial Research (NIDCR). TMJ Disorders: Facts and Statistics. National Institutes of Health. https://www.nidcr.nih.gov/health-info/tmj — Primary source for prevalence data.
-
Calixtre LB, et al. "Manual therapy for the management of pain and mobility in patients with temporomandibular disorder: a systematic review." Journal of Oral Rehabilitation. 2017;44(8):634-652. DOI: 10.1111/joor.12525 — Evidence for manual therapy effectiveness in TMD.
-
American Dental Association. "Evaluation and Management of Temporomandibular Disorders." ADA Clinical Practice Guidelines. https://www.ada.org — Clinical guidelines on splint therapy and first-line TMD treatments.
-
Armijo-Olivo S, et al. "Effectiveness of manual therapy and therapeutic exercise for temporomandibular disorders: a systematic review." Journal of Manipulative and Physiological Therapeutics. 2019;42(4):275-286. DOI: 10.1016/j.jmpt.2019.02.004 — Comparative effectiveness evidence for physical therapy approaches.
-
Klasser GD, Greene CS. "Oral appliances in the management of temporomandibular disorders." Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology. 2009;107(6):834-843. DOI: 10.1016/j.tripleo.2009.01.003 — Evidence base for occlusal splint therapy.
-
Mayo Clinic Staff. "TMJ Disorders: Diagnosis and Treatment." Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/tmj — Clinical overview of TMJ causes and management approaches.
-
American Physical Therapy Association. "PT and TMD: How Physical Therapists Help With Jaw Pain." APTA. https://www.apta.org — Role of physical therapy in TMJ management.
We update this article annually. This page was last reviewed in April 2026. No changes to clinical recommendations were necessary.
About the author: Dr. Rachel O'Neill is a physical therapist specialising in orofacial pain and craniomandibular disorders. She holds a Doctorate in Physical Therapy from the University of Queensland and has worked with patients with TMJ dysfunction in both hospital and private practice settings. Her clinical focus is on combining manual therapy, exercise prescription, and patient education for long-term TMJ management.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified dentist, physical therapist, or medical professional before beginning any new treatment for TMJ pain.